

The Latest
-

Dad, 45, thought he had a pinched nerve in his neck. A rare cancer was to blame
As an employee of the U.S. Postal Service, Len Barchanowicz led an active life and had few health problems. His neck pain was due to an orange-sized tumor.
-

How often should you vacuum?
Experts are weighing in on how often you need to vacuum your floors. The time of year and carpet or hardwood impact how much dirt and grime might be on the ground.
-

Whooping cough outbreak reported at a Montgomery County high school
The Montgomery County Office of Public Health has issued a whooping cough advisory due to an ongoing outbreak at Plymouth Whitemarsh High School.
-
CDC investigating botched Botox shots in 9 states
At least 19 women in nine states reportedly became sick after they got Botox, either having gotten the injections from people who were never licensed or trained to give the shots or received them in “non-healthcare settings,” including homes or spas, the Centers for Disease Control and Prevention said Monday.
-

These foods don't deserve their bad reputations, dietitians and doctors say
Eggs, potatoes, coffee: These kitchen staples, among others, have gained bad reputations, nutrition experts say, but don’t necessarily deserve it. In fact, registered dietitians, doctors and nutrition professors are increasingly advising people to eat them.
-
Experts weigh in on those new health apps promising to help with mind, body and addiction goals
New years resolutions have come and gone. Now that warmer weather is here, lots of people are rekindling those promises to focus on health, diet and wellbeing. One way people are doing that is with the help of artificial intelligence and health apps aimed at improving mind and body functions. NBC10’s Deanna Durante has more from experts on what you... -

Philly college basketball coaching legends Phil Martelli, Fran Dunphy share inspiration for Coaches Vs. Cancer
Fran Dunphy and Phil Martelli join NBC10’s Lucy Bustamante in studio to talk about what inspired them to get involved with t the Coaches Vs. Cancer initiative over two decades ago.
-

As bans spread, fluoride in drinking water divides communities across the US
From Oregon to Pennsylvania, hundreds of communities have in recent years either stopped adding fluoride to their water supplies or voted to prevent its addition.
-
Former Eagle Rodney McLeod, wife back in Philly with Change Our Future Foundation
Rodney McLeod and his wife Erika speak to Philly Live’s Aunyea Lachelle about their plans to host their I am Youth leadership summit in the city.
-
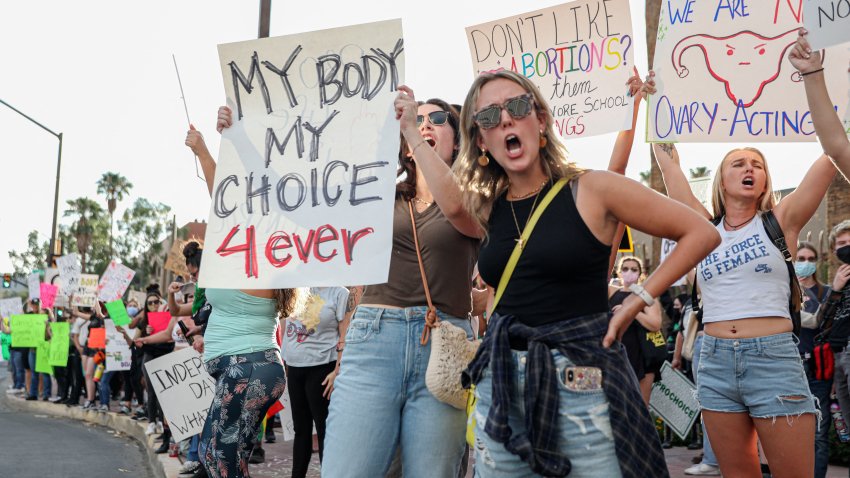
Arizona Supreme Court upholds near-total ban on abortions
The pre-statehood law dates back to 1864 and mandates two to five years in prison for anyone aiding an abortion, except if the procedure is necessary to save the life of the mother.
-
$100,000 grant awarded to Penn Medicine doctor for breast cancer research
A Penn Medicine doctor was awarded a $100,000 research grant to study targeted treatment of an aggressive form of breast cancer.
-
What is eye syphilis? Doctor explains ‘devastating' complication of STD epidemic
As syphilis cases surge in the U.S., few people know the sexually transmitted disease can endanger vision, doctors say.
-

Your spring cleanout could help Cradles to Crayons help kids
Michal Smith, executive director of Cradles to Crayons, joined NBC10’s Lucy Bustamante to talk about children’s clothing insecurity and how people doing so-called “spring greening” can help.







