
- Medicare's annual opportunity to change next year's coverage ends Dec. 7.
- Although experts recommend evaluating your options, most beneficiaries do not review their plan: 67% had not as of mid-November, according to a recent survey.
- Here's what to know.
The clock is ticking: You've only got a few hours left to make sure your 2022 Medicare coverage suits you.
The program's fall open enrollment period, which opened Oct. 15, ends on Dec. 7. While you aren't required to take action — your 2021 plan generally would renew for next year — experts recommend determining whether your current coverage remains your best option.
Nevertheless, most beneficiaries do not review their plan: 67% had not as of mid-November, according to a MedicareGuide.com survey. That's similar to the findings of recent research from the Kaiser Family Foundation, which found 71% do not explore their coverage options during open enrollment.
Get Philly local news, weather forecasts, sports and entertainment stories to your inbox. Sign up for NBC Philadelphia newsletters.
More from Personal Finance:
How to get a jump-start on upcoming tax season
Make these investment moves to beat inflation
More than 1 in 3 U.S. adults carry medical debt
"It can be a really unpleasant surprise for people who think they're happy with their plan and then in January they have to confront the reality that their plan changed, which has an impact on their care or out-of-pocket costs," said Juliette Cubanski, deputy director for Kaiser's program on Medicare policy.
In simple terms, this annual window is for adding or changing coverage related to an Advantage Plan (Medicare Part C) and/or prescription drugs (Part D). You can switch, add or drop those parts of your coverage, and changes go into effect Jan. 1.
Money Report
Fall open enrollment touches most beneficiaries in one way or another due to the coverage they select. For instance, of Medicare's 63.3 million enrollees, 26.7 million choose to get their Part A (inpatient care) and Part B (outpatient care) benefits delivered through Advantage Plans, which are offered by private insurers. These plans are likely to include Part D.
The remainder stick with original Medicare (Parts A and B) and often pair it with a standalone Part D plan. Some also get a Medicare supplemental plan (aka, Medigap), which also is offered by private insurers.
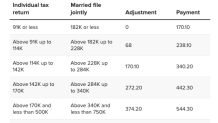
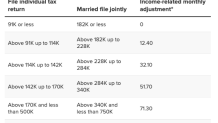
Meanwhile, the standard Part B premium will be $170.10 in 2022, up from $148.50 this year. However, higher earners pay monthly surcharges for Part B and Part D premiums (see charts below).
The average monthly premium for Advantage plans will be $19 next year, down from $21.22 in 2021, according to the Centers for Medicare & Medicaid Services. The average 2022 monthly premium for Part D coverage will be $33, up from $31.47 this year.
Changes to your Advantage Plan could include adjustments to monthly premiums, copays, deductibles, coinsurance or the maximum out-of-pocket limit.
Additionally, "providers may opt in or out of a network plan, or the cost of a prescription drug may be higher or lower, or may no longer be covered," said Elizabeth Gavino, founder of Lewin & Gavino and an independent broker and general agent for Medicare plans.
If you discover after fall enrollment that the Advantage Plan you picked is not a good fit, you can change your coverage between Jan. 1 and March 31. You would be able to switch to either another Advantage Plan or to original Medicare and a stand-alone prescription plan.
However, you would be unable to switch from your standalone Part D plan to another during that early-year window.
Be aware that some Part D plans are folding, said Danielle Roberts, co-founder of insurance firm Boomer Benefits.
"If you're enrolled in a drug plan that's being discontinued, it's likely that your insurance company will [move you] to one of their other drug plans for next year," Roberts said.
In some cases, the other plan may have a significantly higher premium, she said.
"You don't want to find this out in January when it's too late to change your standalone Part D drug plan," Roberts said.






